—
HPI Network > HPI - Health Policy Institute > Health System in Slovakia > 2. Organization and governance > 2.9 Patient empowerment
2.9 Patient empowerment
Wednesday, 04. May 2011, 22:32 — HPI
| << PREVIOUS
2.8 Regulation |
Introduction – Organization – Financing – Resources – Provision – Reforms – Assessment – Conclusions – Appendices |
NEXT >>
3. Financing |
- 2.9.1 Patient information
- 2.9.2 Patient choice
- 2.9.3 Patient rights
- 2.9.4 Patients and cross-border health care
- 2.9.5 Complaints procedures (mediation, claims)
- 2.9.6 Patient participation/involvement
- 2.9.7 Patient safety and compensation
- 2.9.8 Physical access
Advocating patient rights has become a major topic in Slovak health care. To improve the situation, increasing awareness, monitoring and education are important. Currently (2010) there is still no organization to take this forward. Consumer and patient organizations show very different degrees of activity, which is due to their dependence on dedicated individuals and (unstable) external financial funding. Success in advocating for patient rights is often hindered due to the unclear boundaries between the health sector and the social sector, which are both the domain of patient organizations.
2.9.1 Patient information
Information asymmetry is one of the characteristic features of health systems. In spite of the gradual improvement of health system information, explicitly defined information on services covered by SHI, including which diagnostic and therapeutic procedures this may imply, is missing. This creates room for arbitrary interpretation by health insurance companies as well as health care providers.
As far as access to information is concerned, an individual has the right to information on his or her state of health as well as his or her health documentation. Prior to giving informed consent, a condition before a health service can be provided, health care providers must provide patients with all the necessary information.
Health insurance companies provide information on health services performed beyond the coverage of SHI. They are obliged to publish the list of their contracted providers (on the Internet for example). Health care providers have to inform patients in advance if the provided health service is subject to cost-sharing. Physicians have an obligation to inform patients about the co-payment of the prescribed medication and to offer a prescription of a generic with a different co-payment. Patients can verify the pharmaceutical prices and co-payments in pharmacies, since pharmacies must provide an updated list of pharmaceuticals.
Information on quality of providers is scarce. Based on their own analysis, the privately managed health insurance company Dôvera published the first quality assessment of hospitals in 2008, followed by the state-owned General Health Insurance Company later that year.
No institution is actively and systematically monitoring awareness of patient rights or accessibility of information in minority languages. This gap is filled by self-supporting patient organizations.
Although the law guarantees all citizens the right to obtain information from the various public institutions, in practice, frequently there is no data. A survey from 2007 showed that patients mainly rely on family members, friends and the attending doctor when making a choice of health care provider (Fig. 2.5).
Fig. 2.5: Which of the following factors influenced your choice of GP or specialist?
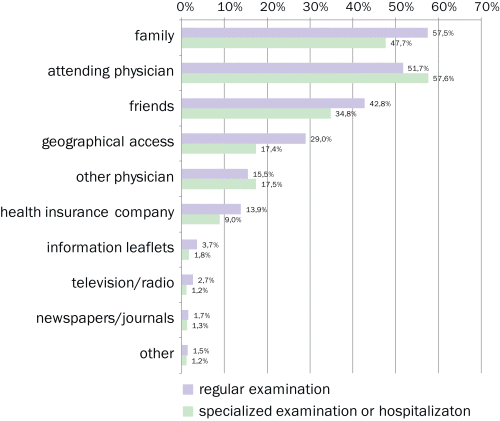
Source: Publicis Knut, 2007.
2.9.2 Patient choice
Free choice in health care encompasses free choice of health insurance company and health care provider, as well as the right to choose a therapeutic procedure.
Free choice of health care provider in SHI is restricted to contractual health care providers, irrespective of where they are based. The list of contractual health care providers is published by health insurance companies. An exception is made for GPs; patients are registered with one GP and can only change their GP once every six months. If an insured person insists on choosing a non-contracted provider, the health insurance company may give an authorization to cover the costs. The providers may not refuse patients except in specified cases, for example work overload or a conflict of interests. Furthermore, providers may decline to perform certain procedures if these are irreconcilable with their religious or other beliefs. If this situation arises, the Chief Physician of the self-governing region identifies a physician who will take care of the patient. If a patient lives in the district where the physician operates, he or she cannot be refused due to work overload. The 2004 health reform gave health insurance companies tools to compete for clients. The insured may change their health insurance company once a year. They can only be refused if they have applied to more than one health insurance company at the same time. Other administrative barriers that could hinder switching health insurance companies (for example, requiring written notice) were removed. Mobility of the insured has varied significantly over time and is influenced by marketing activities and by the extent to which the insured exercise their freedom of choice (Table 2.4).
Table 2.4: Free choice of health insurance company

Patients can decide whether to give informed consent to their health care professionals. In addition, health care professionals are obliged to inform the patients about alternative treatments. When issuing a prescription, the patient may opt for a generic substitution, unless the physician decides that the branded pharmaceutical must be given. Patients have the right to withdraw their informed consent at any time.
The cadaver donation of tissues and organs and autopsies are provided with presumed consent of the donor or autopsied person. Those who wish to protect the integrity of their body after death have to register this in written form at the national register.
The issue of free choice is also frequently associated with abortions. The law on Artificial Termination of Pregnancy of 1986 determines that a pregnancy can be terminated before the twelfth week of pregnancy with prior written application of the pregnant woman. Health care professionals may, based on religious or other beliefs, decline to perform certain procedures related to reproductive health, such as artificial insemination, sterilization or induced abortions.
2.9.3 Patient rights
Awareness of patient rights among patients and health professionals is low. Patient rights in Slovakia are laid down in several acts. The Patients’ Charter (Table 2.5) was elaborated in 2000 as a project of the Ministry of Health, which was funded by the EU’s PHARE programme. It was ratified by Slovakia on 11 April 2001. A group of international and Slovak experts drafted the Charter according to laws in force and international organizations (United Nations, WHO, Council of Europe) cooperated in the project. The goal of the Patients’ Charter was to explain to patients their basic rights in health care. The Charter was approved by the Slovak government in 2001, but the document itself is not legally binding.
Table 2.5: Ten articles of the Patients’ Charter in Slovakia
| I | Human rights and freedom in health care provision |
| II | General patient rights |
| III | Right to information |
| IV | Patient’s consent |
| V | Consent of patients with legal incompetence |
| VI | Confidentiality |
| VII | Treatment and care |
| VIII | Care for incurable and mortally ill patients |
| IX | Complaints submitting |
| X | Compensation of damages |
Source: Patients’ Charter, Government’s resolution No.326 from 11 April 2001.
Furthermore, the European Charter of Patients’ Rights was drafted in 2002 by a European network of civil, consumer and patient organizations called the Active Citizenship Network. The goal of the Charter is to encourage patients to play a more active role in health care provision. This Charter is not legally binding either, but the Network successfully earned recognition in many countries, as well as adoption of rights stated in the Charter. The 2004 Slovak health reform incorporated 14 patient rights from the European Charter into the new reform legislation. Most of the rights from both charters can be traced back to the Council of Europe’s Convention on Human Rights and Biomedicine, which Slovakia ratified in 1999.
Several programmes funded by various grants were used to promote patient rights. Once the funds were exhausted, promotion activities came to an end. The Ministry of Health established a patient rights unit in 2003. The unit provided consultations for patients and information regarding health care provision, as well as monitoring public awareness about observing patients, rights. It was relocated to the HCSA in 2005 and later dissolved. In addition, a non-governmental organization (NGO) called the Association of Protection of Patient Rights deals with patients’ rights.
In spite of declared formal support from the authorities, vulnerable groups of citizens have difficulties advocating for their rights. There are no patient advocates in health care facilities.
Two patient rights issues in Slovakia that have attracted a great deal of international publicity have been net beds (i.e. beds surrounded by nets) used in social and psychiatric care and alleged involuntary sterilization of Roma women.
In 2003, the WHO expressed concern regarding “continuous use of net beds as restricting means in social institutions or psychiatric facilities” (WHO, 2003). According to the WHO, net beds are undignified, humiliating and unsafe. Although net beds ceased to be used in the social sector in 2004, health care facilities continue to use them. The European Committee for the Prevention of Torture visited Slovak psychiatric facilities in 2005. According to the recommendations in their report drafted for the Slovak government, net beds should not be used as a means of getting patients under control. The requirement was unanimously opposed by Slovak psychiatrists. In their view, net beds are used mainly in psychiatric departments as an inevitable instrument for the protection of acute, delirious adult patients and only in cases of unsuccessful psycho-pharmacological treatment. According to the Ministry of Health, there has not been one case of proven misuse of net beds. According to the Committee for the Prevention of Torture, the discussion on net beds with the Slovak government had reached a dead-end. The Ministry of Health did state, however, that a unified form should be drafted to record the indications for and duration of patients’ stay in a net bed in order to prevent the risk of abuse. NGOs signalled cases of alleged involuntary sterilization of Roma women in 2003. Interviews with more than 110 Roma women resulted in the drafting of a report, Body and soul (Center for Reproductive Rights, 2003), which was submitted to the United Nations. Having accepted the report, the United Nations requested an opinion from the Slovak government. According to the report, starting from 1999, Roma women were sterilized for no reason and without prior consent in the hospital in Krompachy and in gynaecology departments of other hospitals. The General Prosecutor’s Office, in cooperation with the Ministry of Health and the Ministry of the Interior, started an investigation. The investigation did not confirm the NGOs’ findings. Sterilizations were performed in accordance with existing legislation. Administrative discrepancies did occur in three cases of under-aged women, on whom sterilization was performed without the consent of their legal representatives. However, sterilization was performed according to the Decree of the Ministry of Health from 1972, according to which sterilization due to health indications does not require informed consent.
As a result, the legislation was amended in 2005 so that informed consent and a completed official application form are prerequisites for sterilization. Furthermore, mandatory instruction on the consequences of sterilization and alternative methods of contraception is required. To sterilize a person who is not legally competent, approval of the court along with the informed consent and a request from his or her legal representative is necessary. This restriction should prevent potential misuse on the one hand, and enables sterilization to be performed in special legitimate justifiable cases on the other. A minimum time of 30 days between submitting the application for sterilization and the procedure itself must be maintained. This time interval reduces the possibility of misuse if a person is making a decision under pressure. It also enables a person to evaluate the situation and offers the chance to withdraw the informed consent in time. Sterilization is an elective procedure (and not urgent care) and the 30-day limit does not endanger a person’s health.
2.9.4 Patients and cross-border health care
Because Slovakia is a Member State of the EU, members of a Slovak health insurance company are entitled to receive services that are covered by statutory insurance in other EU countries, plus Iceland, Liechtenstein, Norway and Switzerland. Based on EC Regulation 1408/71 (now 883/2004), Slovak policy holders can use the European Health Insurance Card (EHIC) to receive health services abroad, paid for by the Slovak system, when on a temporary stay (for example, as tourists). Furthermore, Slovak insured may ask their health insurance company for pre-authorization when planning to receive treatment abroad.
On producing an EHIC, insured Slovaks on a temporary stay abroad and in need of treatment are entitled to reimbursement of health care under equal conditions and equal tariffs as compared to the nationals of another state under the legislation of that state, including financial participation (co-payments). Health care is provided as required so that the insured does not have to return to his country of insurance sooner than intended. The reimbursement does not cover travelling costs. Additional reimbursement is fully in the competence of the health insurance companies.
The conditions for reimbursement of non-urgent (planned) treatment in another state are as follows: (1) pre-authorization by the health insurance company, (2) expected health improvement, (3) lack of treatment possibilities in Slovakia, or (4) insufficient providers’ capacities. In some cases, the health insurance company has the right to identify the health care facility or the state in which the person can seek health care. This applies to the EU Member States as well as countries worldwide. In countries outside the EU the insured may receive reimbursement for urgent health care of the same amount as it would cost in the territory of Slovakia.
In 2007, health insurance companies in Slovakia received 791 applications for authorization of planned health care provision in another EU Member State, of which 743 (94%) were approved. According to HCSA data, since the accession of Slovakia to the EU, there has been a year-on-year increase in the number of people receiving benefits-in-kind abroad. The proportion that the Czech Republic represents in the total of active debts and receivables of Slovakia (47% and 53%, respectively) demonstrates the strong social and professional bonds between the two countries. Table 2.6 shows that especially the number of EU nationals receiving health services in Slovakia has increased significantly over the period 2005–2007, while the number of health services that Slovakians received abroad also increased, albeit this increase is less pronounced. These figures must be interpreted carefully as they may underestimate the true number of people seeking cross-border care. Indeed, they include only those who were treated within the public legal framework provided by EU law or bilateral international agreements. People paying for health care abroad with travel insurance or out-of-pocket payments are not included.
Table 2.6: Number of cross-border health care provision cases and refund claims

To be on the safe side, health insurance companies recommend their insured take out commercial health/travel insurance before travelling abroad. According to a survey on cross-border health conducted by the Gallup Organization (2007), apart from the citizens of Luxembourg (20%) and the Czech Republic (8%), the Slovaks (7%) belong to the most frequent users of health care in the EU Member States in 2007. Fifty per cent of Slovaks have expressed willingness to travel abroad to seek health care. From treatment abroad, the Slovaks expect higher quality (87%) and help from a renowned specialist (83%). Satisfaction with health care in Slovakia (72%) is higher than the average in other EU12 Member States (59%), but lower than the average in EU15 Member States (89%) (see Table 2.7).
Table 2.7: Factors motivating patients to obtain medical treatment in other EU Member States, or discouraging them (%) in Slovakia, EU12, EU15 and EU27

Spa treatment and orthopaedic services (total endoprothesis, arthroscopy) are traditionally the most sought health care services in Slovakia, mainly for patients coming from Arab countries. Considering the relatively low prices of dental care, an increased demand for dental services has been observed. Also for in vitro fertilization an increased demand from countries with stricter regulation of reproductive health (Italy, for example) is observed.
2.9.5 Complaints procedures (mediation, claims)
When patients or their relatives presume that a health care service was not adequately provided they can submit a written complaint to the health care provider. If a health care provider does not satisfy this appeal, it is the patient’s right to request the HCSA to assess whether adequate health care was provided. Other complaints (for example, regarding user fees, ethics, and organization of health care) must be submitted to the relevant body (for example, the Ministry of Health, self-governing regions, professional chambers). The law prohibits persecuting a person who is exercising his or her right to file a complaint, claim or start a criminal prosecution against a health care professional or provider.
The HCSA, as an independent body for monitoring health care, has become a credible advocate of patient rights. The HCSA annual reports on health insurance performance include information on the composition of patients’ complaints (Table 2.8). In cases of a violation of the law, the HCSA can impose different sanctions and proposals for remedy measures. Surgery was the specialization most penalized in 2008 (42 cases). The total number of cases giving rise to trials submitted by the HCSA in 2008 was 6, which was lower than the preceding years (30 in 2006, 9 in 2007).
Table 2.8: Main causes of cases filed in relation to provided health care
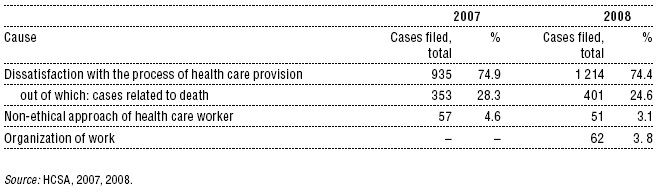
The HCSA handles the complaints of patients concerning health insurance companies (Table 2.9). The complaints concern, for example, unfair practices in recruitment of the insured by two private health insurance companies (suspicious application submission for switching health insurance companies, misuse of personal data, application submission based on misleading information).
Table 2.9: Patients’ complaints and motions regarding individual health insurance companies, 2007a

2.9.6 Patient participation/involvement
Patients’ participation in formal decisions in health care is very limited. Representing organizations and associations have an opportunity to comment on new legislation, but they can only make recommendations. They are too fragmented and frequently lack adequate funding. Patient organizations can advocate for their interests by lobbying legislators and by influencing public opinion. By allowing real competition in health insurance the insured have the possibility of influencing purchasing policy indirectly. Negative publicity surrounding complaints may result in an outflow of insured, which motivates health insurance companies to make a settlement.
So far, surveys on patients’ satisfaction with providers are rare. They are mainly conducted by health insurance companies. Two health insurance companies (the state-owned General Health Insurance Company and privately owned Dôvera) published their results and used them as one of the criteria when purchasing health care services in 2008. In general, the level of satisfaction with providers was evenly spread. The results of the patients’ satisfaction survey in 2008 indicated that patients consider the level of additional (hotel) services less satisfactory than the quality of health care (Table 2.10).
Table 2.10: Patients’ satisfaction survey, 0 (lowest) – 100 (highest)

2.9.7 Patient safety and compensation
Apart from the reporting of adverse drug reactions, risk reduction of iatrogenic harm to patients is not subject to legislation. Health care providers are obliged to have liability insurance for damages related to health care provision to patients. Liability insurance is provided by commercial insurance companies.
Filing an appeal to health care facilities or physicians for compensation for non-financial damage is uncommon. The amount of required financial compensation for unsuccessful operations or death due to negligence is rarely more than €100 000. To receive compensation a patient is advised to submit a complaint to the HCSA. The HCSA will then start an investigation. If the law was violated, the claimant has the burden of proof in a civil legal dispute with a health care professional. A health professional cannot be exempted from this liability. Criminal prosecution is considered only if a health professional has committed a crime according to the definition of Criminal Law. This applies to crimes against life and health. No intentional cases have been reported in the past 15 years; only cases of crime due to negligence have been reported (reckless homicide, harm to health, withholding aid).
Since 2005, the HCSA has been publishing case reports of irregularities with health care providers, most of them with a tragic end. According to evaluation by experts, the failures concerned timely and correct diagnosis, or treatment procedures. The most severe cases are evaluated by an expert committee of the Chair of the HCSA. The case reports help to extend the education of health professionals and are intended to promote patient safety by preventing such situations.
Advertising of private practices, health care facilities and diagnostic and therapeutic procedures is allowed. As stated in the Ethical Codex of a health care professional, the advertisement should be moderate, informative and should not bear signs of unfair competition. The advertising text and its publicity should not discredit the health care professional. For pharmaceutical regulation aimed at protecting patients (for example, pharmacovigilance and advertising), see section 2.8.4 Regulation and governance of pharmaceuticals.
2.9.8 Physical access
A Ministry of Health decree obliges both outpatient and inpatient health care facilities to ensure a barrier-free environment for patients with restricted movement and orientation. Patient organizations claim that this is not in accordance with reality and keep expressing the need for action. A conflict of competences and a lack of coordination between the Ministry of Health and the Ministry of Social Affairs is a barrier to an effective solution. The agenda of people with special health care needs is the competence of the Ministry of Social Affairs. This Ministry lacks some of the needed competences in health care to effectively solve the situation. Therefore, organizations of people with disabilities have been lobbying for the adoption of the revised European Social Charter. Article 15 of this Charter binds the subscribers to provide technical support in order to overcome barriers in communication and movement.
In 2004 and 2005, the Slovak Union of People with Physical Disabilities (2005) conducted a nationwide survey on the accessibility of public buildings. The survey indicated a higher proportion of barrier-free buildings and better accessibility in general in the Bratislava region as compared to more rural areas. Physical access was also one of the parameters evaluated within the rating of health insurance companies in 2008. None of them met the condition of a barrier-free environment during mystery shopping (Szalayová et al. 2008).
Lastly, new buildings and renovated existing buildings are obliged to ensure that there is barrier-free access. Organizations of people with disabilities report increased requests for their consultations from investors and contractors.
News
The amendment of the Decree on emergency medical service
Health insurance companies returned over 400 thousand €
The HCSA received 1,647 complaints last year
A half million people will earn more
Most of public limited companies ended in the black
Debt of hospitals on premiums has grown to nearly € 105 MM
Slovak health care may miss € 250 million next year
Profits of HIC amounted to € 69 mil. last year
Owners of Dôvera paid out money but did not paid taxes
Like us on Facebook!
Our analyses
- 10 Years of Health Care Reform
- New University Hospital in Bratislava
- Understanding informal patient payments in Kosovo’s healthcare system
- Analysis of waiting times 2013
- Health Policy Basic Frameworks 2014-2016
- Analysis of informal payments in the health sector in Slovakia
- Serbia: Brief health system review
developed by enscope, s.r.o.
