—
HPI Network > HPI - Health Policy Institute > Health System in Slovakia > 7. Assessment of the health system > 7.3 Efficiency of resource allocation
7.3 Efficiency of resource allocation
Friday, 06. May 2011, 20:30 — HPI
| << PREVIOUS
7.2 Equity |
Introduction – Organization – Financing – Resources – Provision – Reforms – Assessment – Conclusions – Appendices |
NEXT >>
7.4 Technical efficiency |
According to OECD Health Data (2010a) an international comparison of the Slovak health system shows that (see also Table 7.4):
-
Health spending per capita in Slovakia (US$ 1738 per • capita in PPP) is half of the EU15 average (US$ 3483), on the same level as in the Czech Republic (US$ 1 781), 20% higher than in Hungary (US$ 1 437) and 40% higher than in Poland (US$ 1 213).
-
Hospital bed availability (6.6 beds per 1000) is, with Poland, the lowest among the Visegrád Four countries, but higher than for the EU15 (5.3) and OECD (5.6). However, the acute care occupancy rate (67.5%) is the lowest among the Visegrád Four and significantly lower than for the EU15 (76.4). On the other hand, discharge rates (20.8 per 100) are the highest among the Visegrád Four and 20% higher than for the EU15 (17.3).
-
The number of consultations (12.1 per capita) is only slightly higher than in the Czech Republic (11.4) and Hungary (11.3), but almost double that of Poland (6.8), the EU15 (6.7) or OECD average (7.7).
-
Spending on pharmaceuticals in Slovakia (US$ 489 per capita in PPP) is at the same level as the OECD (US$ 490) and much higher than in Hungary (US$ 454), the Czech Republic (US$ 363) or Poland (US$ 274). Combined with the lower economic performance of Slovakia (US$ 22 193 per capita in PPP) compared to the OECD average (US$ 33 271) this means that pharmaceutical expenditure in Slovakia is 2.2% of GDP compared to 1.5% GDP in the OECD, or 28% of total health care spending versus 16% in the OECD.
-
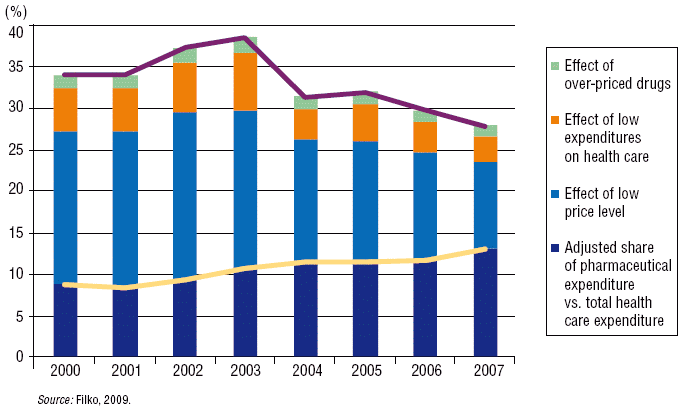
According to Filko (2009), high spending on pharmaceuticals in Slovakia (Fig. 7.3) can be explained mainly by the effect of the low price level for health services in Slovakia (which makes pharmaceuticals relatively expensive), to a lesser extent by the lower level of other health care expenditure and, finally, to a small extent, to the effect of over-priced drugs (Fig. 7.4). The high proportion of expenditure on drugs leaves only a little room for growth in outpatient and inpatient care. Experience from recent years shows that more resources can be allocated to inpatient and outpatient care when drug expenditure is not rising quickly.
Table 7.4: Selected health resources, 2008
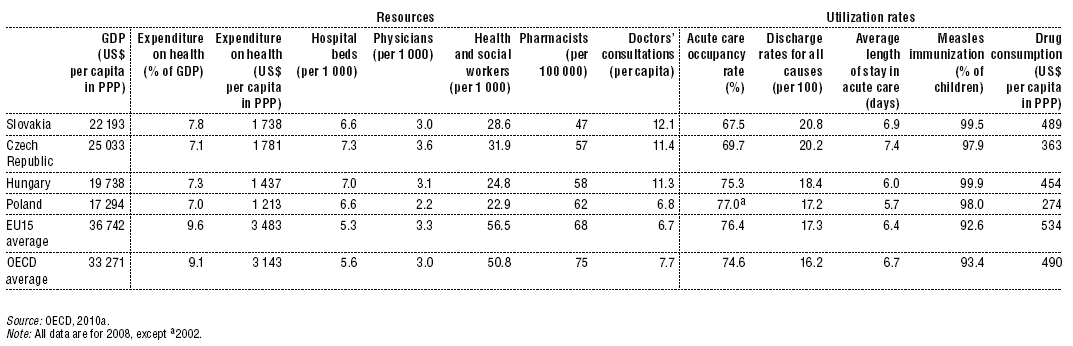
Fig. 7.3: Pharmaceutical expenditure in Slovakia vs OECD and Visegrád Three (Czech Republic, Hungary, Poland) as % of total health expenditure
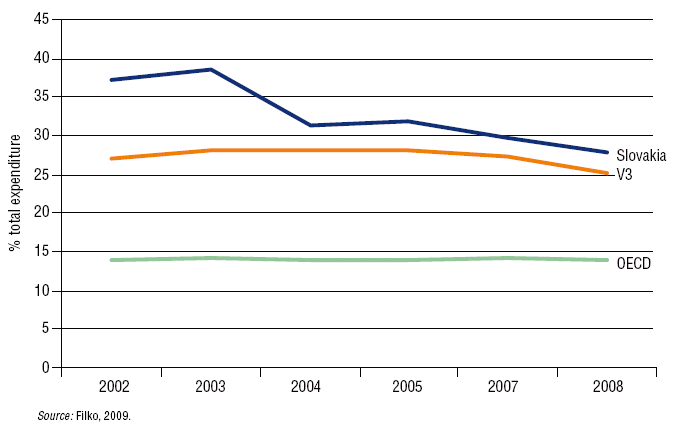
Fig. 7.4: Components of pharmaceutical expenditure in Slovakia
The OECD Health Data (2010) also shows that health outcomes in Slovakia are relatively close to the other three Visegrád Four countries but significantly worse than the averages for the EU15 and OECD (see Table 7.5):
-
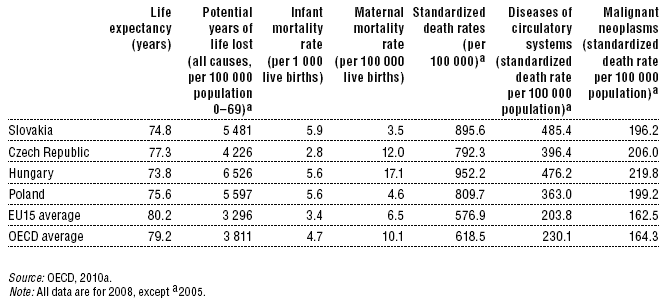
Life expectancy in Slovakia is 74.8 years, five years less than the EU15 (80.2 years) and OECD averages (79.2 years).
-
The standardized death rate (895.6) is 55% higher than the EU15 average, while the standardized death rate for diseases of the circulatory system (485.4) is the highest among the Visegrád Four countries and more than double the EU15 (203.8) and OECD (230.1) averages. In contrast, the standardized death rate for malignant neoplasms is the lowest among the Visegrád Four countries and only 20% higher than the EU15 (162.5) and OECD (164.3) averages.
-
Infant mortality in Slovakia (5.9 per 1000 live births) is slightly above the level of Hungary and Poland (both 5.6) and significantly higher than the EU15 average (3.4). On the other hand, the maternal mortality rate is significantly lower in Slovakia (3.5 per 100 000 live births) than the EU15 (6.5) or OECD (10.1) averages.
Table 7.5: Health outcome in the Visegrád Four, EU15 and OECD
These observations are in line with a 2007 IMF study (Verhoeven, Gunnarsson & Lugaresi 2007), which concludes that Slovakia, like other EU10 countries (i.e. the 10 countries that joined the EU in May 2004), combines relatively low health spending with relatively poor health outcomes. Inefficiencies in the Slovak health system occur mostly in the process of transforming intermediate health resources into health outcomes. The IMF study sees two reasons for this. First, this is due to inertia – for instance, hospital structures may still reflect old standards and a significant proportion of current health workers were educated in the pre- and early transition period. Second, high cost–effectiveness in Slovakia reflects relatively low prices for labour and other inputs for health services. As a result, despite spending levels, real resources in the health sector are relatively high.
News
The amendment of the Decree on emergency medical service
Health insurance companies returned over 400 thousand €
The HCSA received 1,647 complaints last year
A half million people will earn more
Most of public limited companies ended in the black
Debt of hospitals on premiums has grown to nearly € 105 MM
Slovak health care may miss € 250 million next year
Profits of HIC amounted to € 69 mil. last year
Owners of Dôvera paid out money but did not paid taxes
Like us on Facebook!
Our analyses
- 10 Years of Health Care Reform
- New University Hospital in Bratislava
- Understanding informal patient payments in Kosovo’s healthcare system
- Analysis of waiting times 2013
- Health Policy Basic Frameworks 2014-2016
- Analysis of informal payments in the health sector in Slovakia
- Serbia: Brief health system review
developed by enscope, s.r.o.
